Author: Sofia Ruiz-Sierra
Editors: Chloe Rybicki-Kler, Emily Eberhardt, & Madeline Barron
Illustrator: Jacquelyn Roberts
Imagine a world where doctors had no way of measuring blood pressure. They would have a hard time determining how hard your heart is working or whether you were at risk for serious conditions, like heart disease or stroke. Blood pressure is an example of a biological marker, or biomarker. Simply put, biomarkers provide insights into your health status.
Similarly to how blood pressure serves as a biomarker for heart health, biomarkers may also be critical in understanding psychotic disorders, such as schizophrenia. These biomarkers would allow researchers to obtain objective and reproducible measures to prevent, diagnose, and treat psychotic disorders. Providing an accurate diagnosis to patients increases their opportunities for early treatment and improved prognosis. However, identifying reliable biomarkers that allow scientists to understand and quantify complex cognitive disorders is complicated, as results are often inconclusive. Nevertheless, over the past decade, a brain protein called the Brain Derived Neurotrophic Factor (BDNF) has emerged as a potential biomarker for cognitive deficits in psychotic disorders.
What is BDNF?
BDNF is a protein that plays a role in the growth, differentiation, and maintenance of neurons. It is mainly active at the synapses, the space between neurons where cell-to-cell communication occurs, and is necessary for the maintenance and formation of functional synapses. BDNF is also involved in the cellular mechanisms underlying cognitive functioning (i.e., the ability to speak, learn and remember information, make decisions, and solve problems). As a result, altered BDNF levels have been associated with cognitive deficits, a core manifestation of psychotic disorders.
Given its role in these neuronal processes, scientists have proposed altered BDNF levels as a biomarker of cognitive impairment in psychotic disorders. However, scientists have primarily studied BDNF levels in chronic schizophrenic patients, virtually excluding those who are undiagnosed but may experience psychotic symptoms like hallucinations and delusions. Investigating BDNF levels in those who are at risk of developing psychotic disorders and those who have experienced their first episode of psychosis (FEP) is critical, as it may provide insight into the progression of psychosis. Early detection of altered BDNF levels may even lead to an early diagnosis and treatment of these disorders.
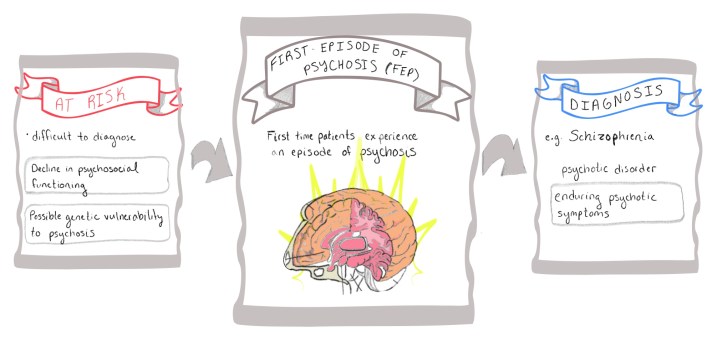
A broader understanding of the BDNF-psychosis link
To that end, researchers have recently begun to place greater emphasis on individuals at high risk of psychosis as well as FEP patients when investigating the intersection between BDNF levels and psychosis. Together, these two newly-investigated stages of psychosis indicate a shift in researchers’ interest. That is, instead of restricting research of BDNF as a biomarker of cognitive impairment to patients with chronic schizophrenia, those who display early symptoms of psychosis may also benefit from this research!
While expanding research on BDNF to earlier stages of psychotic disorders is ideal, it also poses a new challenge. That is, how are abnormal levels of BDNF quantified? After all, biomarkers are objective, reproducible measures. For the most part, studies report lower levels of BDNF in subjects at high-risk for schizophrenia and FEP patients compared to control groups, though studies of this nature are still scarce.
Research also suggests a positive association between blood plasma BDNF concentrations and cognitive functioning, including increased perception, memory, learning, attention, decision making, and language abilities. This evidence suggests that increased levels of plasma BDNF correlates with improved cognitive functioning! Consistent with this finding, new evidence suggests a correlation between low serum BDNF levels and reduced volume of the hippocampus, a region of the brain linked to cognitive functioning, at the onset of psychosis. Together, these studies suggest that reduced BDNF levels may lead to cognitive deficits, an important predictor of psychosis.

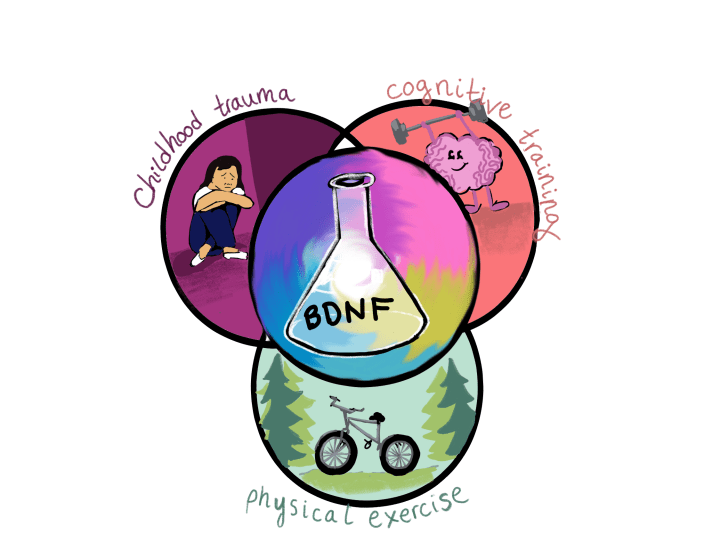
As researchers continue investigating BDNF levels in high-risk and FEP patients, recent findings suggest that this brain protein may also serve as a biomarker in other contexts. For instance, BDNF may play a role in the onset of psychosis in individuals exposed to childhood trauma. This means that BDNF could also be a possible biomarker for the detrimental effects of childhood trauma on the brain!
Additionally, BDNF levels may also be informative of the efficacy of non-pharmacological treatments in patients with chronic schizophrenia. In two studies, BDNF levels were increased in patients participating in non-pharmacological interventions like cognitive training. This form of treatment focuses on improving cognitive functioning by assigning patients with structured tasks designed to train cognitive processes like attention, memory, or problem solving. BDNF levels may allow researchers to objectively assess improvements following these treatments. As a result, non-pharmacological interventions could present an alternative to the use of antipsychotic drugs–often the only option for the treatment of psychotic disorders. At the same time, alternative treatments like cognitive training may benefit patients in all stages of psychotic disorders, including at-risk and FEP patients. However, there is still much controversy regarding their usefulness and applicability in clinical practice.
There is also growing interest in the effects of physical exercise on BDNF levels; studies report patients with schizophrenia showed significant increases in their BDNF levels and improved performance on cognitive tests after aerobic exercise (e.g., active-play video games or traditional cardiovascular exercise). Different molecular mechanisms have been proposed to explain how physical exercise enhances BDNF synthesis in neurons, though no definitive conclusions have been reached. Nevertheless, this association demonstrates the importance of investigating the effects of BDNF on cognitive function.
Moving forward
Now, where does this leave us? While it is critical to recognize and bring attention to the advancements made in the field in recent years, it is equally important to peek at the future of BDNF. Today, there are still no reliable biomarkers to monitor therapy efficacy or to aid diagnosis of psychotic disorders. However, as recent research points out, BDNF might be the answer we are looking for. Further research on BDNF as a biomarker of cognitive impairment is necessary to provide a reliable and early diagnosis to those who have, or are at risk of developing psychotic disorders. Not only would this lead to early treatment, but also to improved prognosis. While studies of this nature have begun to appear, they are still scarce and have limited sample sizes. Nevertheless, with targeted efforts from the scientific community and funding toward this important quandary, important developments into the field can be made.

Sofia Ruiz-Sierra (she/her/ella) is a first-year undergraduate student in the Biopsychology, Cognition and Neuroscience department currently investigating methodological challenges of using DNA methylation on stress-related genes as biomarkers of stress. She is passionate about science, film, and baking shows and would love to see more latinx women in STEM.
