Author: Lei Wan
Content Editor: Zena Lapp, Kristina Lenn; Senior Editor: Sarah Kearns
Disclaimer: The opinions in this post belong to me. Patients should consult their own physicians about what will work best for their treatment and recovery plan.
When I volunteered in a cooking class for cancer patients and cancer survivors, I was often asked about nutrition and dietary supplement choice. For example, patients with colon cancer would ask if they should take omega-3 fatty acids; patients with prostate cancer were interested in taking lycopene and vitamin E. I pondered the same questions when my mom was diagnosed with breast cancer and when her cancer recurred—would she recover faster if she ate more cruciferous vegetables like broccoli and Brussels sprouts? These questions are also of interest to the public, given increasing evidence supporting the role of nutritional factors in cancer development.
Cancer is a chronic disease characterized by uncontrolled cell growth. The majority of cancers are not inherited or passed down. Rather, cancer is the result of the accumulation of damage and changes to the gene in cells over time. The damage and changes can be caused by both internal and external factors. Internal factors are related to systems within the body and include inherited genetic mutations or abnormal immune function. External factors are factors outside of the body. They can be categorized into environmental factors such as radiation and viruses and lifestyle factors such as smoking, diet, nutrition, and physical activity.
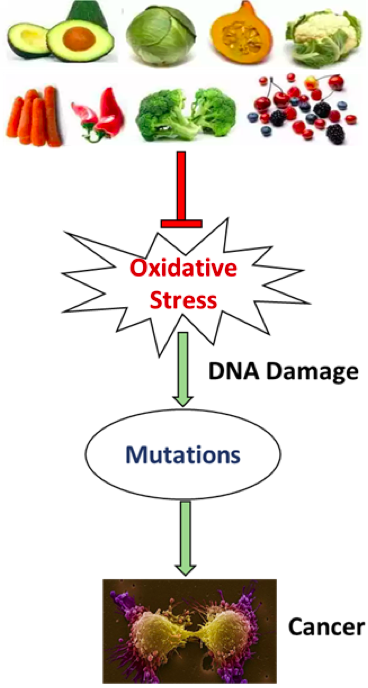
External factors influence the regulation of gene expression, leading to genetic mutations and eventually cancer over a long period of time. For example, environmental factors such as smoking and lifestyle factors, such as a high-fat diet, stress cells and induce oxidative stress. Oxidative stress leads to DNA damage and contributes to cancer formation
What is oxidative stress? When cells burn nutrients and oxygen to produce energy, they produce a by-product—reactive oxygen species (ROS). ROS can easily react with DNA, lipids, and proteins, leading to cell membrane and tissue damage. The human body has a defense system–certain enzymes and antioxidants–to remove excess ROS and maintain a balanced state between production and removal of ROS. Oxidative stress occurs when there is imbalance towards ROS.
How does nutrition modify cancer risk?

Nutrition provides what we need to grow, reproduce, and be healthy. The importance of nutrition was accepted after scientists found that specific foods could prevent certain diseases. For example, scurvy can be prevented by a diet with lime (vitamin C) and beriberi can be prevented by a diet with evaporated milk and meat (thiamin/vitamin B1). Numerous studies suggest that nutrition also influences cancer development.
The relationship between nutrition and cancer has been studied in large population-epidemiological studies. These studies examined if disease incidence is influenced by environmental or lifestyle factors. As early as 1981, a review of available epidemiological studies indicated that different cancer rates can be attributed to external factors including smoking and diet. Following this landmark study, numerous studies observed that people who eat a lot of vegetables and fruits have lower cancer risk, whereas people who consumed more red and processed meat have increased cancer risk. These studies demonstrated the critical roles nutrition may play in cancer development.
Further, these observations stimulated experimental analysis to identify food and food components that are responsible for cancer-altering effects. Fat is one of the first nutrients shown to have effects on cancer development. Specifically, caloric restriction inhibits tumor growth and increased fat intake promotes cancer formation, especially in hormone-dependent cancers such as breast and prostate cancer. Types of dietary fat also matter. While trans-fat seems to be cancer-promoting, polyunsaturated fat (omega-3 unsaturated fatty acid) seems to inhibit cancer cell growth. Moreover, researchers have shown that particular vitamins (vitamin C, D, and E) and minerals (calcium and selenium) inhibit cancer growth in cell culture and mouse models.
Many food components are not nutrients but still have effects on health and cancer development. They are called bioactive compounds. For example, lycopene, the pink pigment in tomato, inhibits prostate cancer growth. Many anti-cancer bioactive compounds were identified in broccoli, black raspberry, curcumin, and soy. These food components are potent antioxidants. They reduce ROS-induced DNA damage and cancer formation. These laboratory findings fuel clinical examination of the effects of nutrients and bioactive compounds in patients with cancer.
Issues in nutritional studies
When food constituents found to reduce cancer risk in mouse experiments were tested in clinical trials, most studies failed to reproduce what was previously found. Some studies even indicated harmful effects of these compounds. For example, both vitamin E and beta-carotene were shown to reduce cancer risk in animal models, but a human study in Finland showed that daily beta-carotene supplement may increase lung cancer risk in smokers. Additionally, in 2011, an international study with about 36,000 subjects reported that intake of vitamin E increases prostate cancer risk in healthy men.
These controversies create misleading information about the role of nutrition in cancer development and reveal shortcomings in nutrition research. Conventional nutritional research uses reductionist methods that attempt to attribute the beneficial effect to a single food component. This approach has two potential pitfalls.
First, this method fails to consider the interconnectedness of food components. For example, spinach is a rich source of vitamin A, vitamin C, and vitamin K, which are all considered strong antioxidants and anti-cancer agents. Epidemiological studies try to identify the key food component that reduces cancer risks among all the contributors. As a result, the single component identified is hard to interpret which, in part, accounts for the negative results of human studies.
Second, the amounts of food components used in either laboratory or clinical research are much higher than the levels consumed in a typical diet. The investigated food constituents are antioxidants and reduce ROS, but because they are used in such high concentrations, this might cause damage. Although ROS are carcinogenic, they also induce cell death and can remove cancerous cells. Therefore, it is possible too many antioxidants, by delaying or inhibiting cell death, favors the survival of precancerous cells. This hypothesis was confirmed in a study in which vitamin E reduced ROS-induced DNA damage yet increased tumor cell proliferation in a mouse model.
Importance of dietary pattern
The limitations of reductionist methods have stimulated research on how dietary pattern, instead of single nutrients, influences cancer risk. Dietary pattern is what, how much, and how often we eat and drink. The study of dietary pattern focuses on the complete composition of consumed food and drink. It studies connectivity of food components at levels consumed in a typical diet. So far the dietary pattern with reduced fat and increased fruit and vegetables has been confirmed to improve relapse-free survival and reduce mortality in patients with breast cancer. Currently, one trial examined the effect of a diet rich in vegetables and fruits in breast cancer recurrence and did not show a statistically beneficial effect of the diet. More trials are required to define the role of certain diets in cancer treatment and survivorship.
Considering all the available evidence including epidemiological, laboratory, and clinical studies with a rigorous scientific process, the World Cancer Research Foundation/American Institute for Cancer Research (WCRF/AICR) recommends that people consume a balanced diet consisting of vegetables, fruits, and limited red and processed meats for cancer prevention and survival. Moreover, WCRF/AICR emphasizes a healthy weight range and physical activity. In contrast, dietary supplements such as vitamin E and beta-carotene are not included in the recommendation. This recommendation is also echoed by other organizations including the American Cancer Society and the European Society for Clinical Nutrition and Metabolism.
If you are a cancer patient or a caregiver for patients with cancer, studies support monitoring diet and nutrition during and after treatment. A balanced diet—low fat and rich in nutrients and bioactive compounds that have anti-cancer activities—seems to be beneficial, and includes things like olive oil, broccoli, tomatoes, and black raspberries. Should you take a dietary supplement to prevent cancer or improve cancer treatment? Based on the current findings, the answer is likely no. In the future, there may be scientific evidence supporting the intake of dietary supplements. But for now, the evidence suggests that consumers should focus on a healthy and balanced dietary pattern instead of single food components.
 Lei is a postdoctoral fellow in the Translational Oncology Program at the University of Michigan. Her research focuses on targeted therapy development and drug resistance in aggressive breast cancer. She received her Ph.D. in Nutritional Sciences at The Ohio State University. Besides science, she enjoys doing ballet and yoga.
Lei is a postdoctoral fellow in the Translational Oncology Program at the University of Michigan. Her research focuses on targeted therapy development and drug resistance in aggressive breast cancer. She received her Ph.D. in Nutritional Sciences at The Ohio State University. Besides science, she enjoys doing ballet and yoga.
Read more by Lei here.

Such a great post and so important! Prevention over prescriptictions…being proactive rather than reactive with our health… improving our lifestyle! amazing.
LikeLike