Author: Shannon Wright
Editors: Ellyn Schinke, Jessica Cote, Alisha John
What is the most deadly virus in the world? The answer may surprise you. If we consider case fatality rate (the number of people infected who die from the virus if left untreated), it’s not Smallpox (20-60%), or even the Ebola virus (~50%), but rather, a common mammal-targeting virus you almost certainly have heard of: rabies. With no known cure, this infamous virus has a 100% fatality rate – certainly worthy of a gold-medal if we were giving out medals for how deadly viruses are.
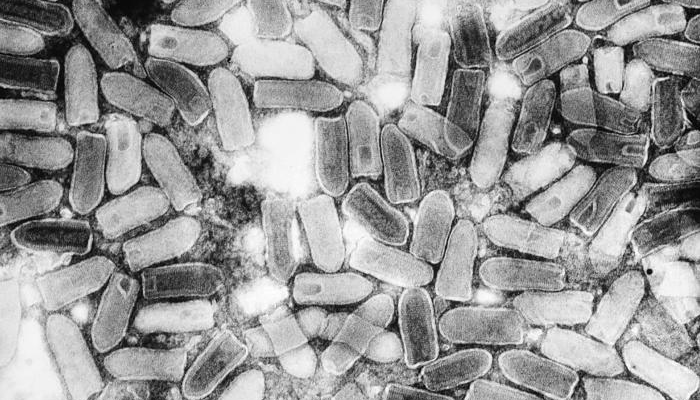
Figure 1: The rabies virus is a member of the Rhabdoviridae family, with a characteristic “bullet” shape.
Most people in the U.S. who do get rabies are infected from their pets like domesticated dogs and cats, through their bite. But human cases of rabies in the U.S. are rare, with one to three cases reported annually. If the virus is so deadly, why don’t more people die from rabies? It turns out that our best defense is a good offense. The Center for Disease Control and Prevention suggests that individuals who are bitten by a wild animal or potentially exposed to rabid animals begin the series of vaccinations against rabies immediately. Unlike for most vaccinations, for rabies, vaccination occurs after a potential exposure.
The rabies vaccination consists of dead viruses that will not cause the illness. The immune system recognizes the dead viruses as foreign objects and begins to mount an immune response, giving the immune system a head start on battling the live virus. In other words, the vaccine speeds up the natural immune response against the live virus and helps your body rid itself of the virus before it can reach the central nervous system (the brain and spinal cord).
A typical course of rabies immunization involves four vaccine doses given over the course of two weeks, often costing more than $3,000. The vaccination is a highly effective treatment for rabies infection, but people may not seek medical attention in the absence of symptoms. Additionally, pursuing the proper medical treatment for a potential rabies infection proves difficult for those with limited access to medical facilities or for those whose insurance does not cover the vaccination. To others, a superficial bite wound may not seem serious enough to warrant a doctor’s visit.
What Makes Rabies Virus So Deadly?
In the cases where the vaccine is not administered before symptoms arise, what is it that makes the rabies virus so difficult to combat? The most effective viruses have a “get in, get out” policy. The rabies virus is a prime example, as it is highly infectious (“get in”) and easily transmissible (“get out”). To “get in”, the rabies virus enters the muscle at the site of the bite and enters a nearby nerve. The virus then travels the length of the nerve and crosses the spaces between neurons, known as synapses, to reach the central nervous system. Only then, after the virus has reached the central nervous system, the virus begins to replicate. This process can take weeks – which is what allows the vaccination to be effective after exposure.
After replication, the virus travels back out into the nerves, causing characteristic rabies symptoms such as paralysis and excess saliva production. As soon as symptoms become evident, administration of the vaccine no longer prevents the disease. By lying under the radar until it is too late to treat, the rabies virus evades one of modern medicine’s most basic tools for diagnosis and disease prevention: the presence of symptoms. This way, the rabies virus increases its likelihood of successfully infecting a host by evading detection until it is untreatable. Therefore, it is essential to receive the vaccine after potential rabies exposure even in the absence of symptoms to prevent onset of the disease.
To enhance its ability to “get out”, the rabies virus manipulates its host physically and behaviorally to improve its chances of transmission from the primary host to new hosts. One of the most interesting symptoms caused by rabies that might help with the transmission is hydrophobia (‘fear of water’) – in which rabies patients show panic when presented with liquids. This aversion to drinking leads to difficulty of swallowing and excess production of saliva – together causing the classic rabies symptom of foaming at the mouth. The excessive saliva production also ensures that the host has plenty of virus-containing saliva ready to enter a new host.
But how will the virus be transmitted to the new host? Rabies increases agitation resulting in the typical “rabid” behavior, including increased aggression and a propensity to bite and spread infection. These symptoms ultimately transform the host into a ready and willing vehicle of transmission, increasing the likelihood that its host will spread the virus to others. While rabies is not typically transmitted from human-to-human, human patients still exhibit these aggressive behaviors. In humans, the rabies virus causes anxiety, confusion, agitation and hallucinations, increasing the host’s aggression.
A Case Study: Jeanna Giese
Rabies is a brilliant virus that exploits the host for self-propagation while still killing every one of its victims…almost. Let’s examine the case of Jeanna Giese, who was bitten by a bat when she was 15 years old. Although her parents cleaned the wound, the bat’s saliva entered her bloodstream and the rabies virus in the bat’s saliva attacked the nearby nerves. After this initial infection, the virus laid below the radar for 37 days, producing no symptoms until it reached the central nervous system. At this point the symptoms including fatigue, double vision, vomiting, and tingling in her left arm arose, seemingly condemning Jeanna to an almost certain death. But Jeanna survived.
In most cases, the rabies virus can only be defeated upon administration of the vaccine. However, there is a very small portion of the population, who survive rabies infection without vaccination, possibly possessing an enhanced immune response that allows them to defeat the disease. Jeanna Giese is likely one of these rare individuals, being one of only three people in the United States known to have survived a rabies infection without receiving the vaccination. Dr. Rodney Willoughby, Jr. treated her by chemically inducing a coma while administering antiviral drugs, believing this regimen would provide her immune system time to catch up with the virus. This experimental treatment, known as the Milwaukee protocol, has worked in Jeanna but failed in other patients, suggesting that there is something different about these individuals. Maybe Jeanna had an enhanced immune system compared to other patients, but the Milwaukee protocol may be a place to start to research for a cure for rabies.
What’s Next for Rabies Research?
While there is still no cure for rabies, the current policy of post-exposure (or post-potential exposure) vaccination eliminates the rabies virus as a major public health problem in the U.S. due to the effectiveness of the vaccine. However, the rabies virus is still a significant global health issue since it kills more than 59,000 people every year, mostly in Asia and Africa, and disproportionately affecting children under the age of 15. In the U.S. alone, an estimated 40,000 people annually receive the rabies vaccination, totaling a U.S. public health cost upwards of $500 million.
The high cost of rabies vaccine can be prohibitive. There are many approaches we can take to stop rabies abroad and decrease the U.S. public health cost. First, as dogs are the most common source of rabies spread to humans, and vaccination of dogs dramatically reduces the occurrence of rabid animal bites, more efforts to ensure canine vaccination in the U.S. and abroad would help alleviate the health and financial burden of rabies. Secondly, development of an effective test for rabies infection would reduce the number of preventative vaccinations administered annually. Lastly, by spreading awareness of the disease and its signs in animals, we would encourage people to seek life-saving medical attention in the case of an animal bite before it is too late.
Rabies may be a gold-medal virus, but with increased awareness and improved preventative practices, we can leave it in the dust.
About the author

Shannon Wright is a PhD student at the University of Michigan in the Neuroscience Graduate Program. Originally from Rochester, New York, Shannon graduated from Kenyon College in Gambier, Ohio with a degree in Biochemistry and Neuroscience, where she studied Polymer Chemistry. At UM, she investigates mechanisms of synaptic plasticity and neurodegeneration. To read all posts by Shannon, click here.
Image Sources:
Figure 1: http://myplace.frontier.com/~dffix/medmicro/pix/rhabdo.png

Best of luck for next research
LikeLike
Why is there a prophylactic vacine for dogs and cats and not for humans? What is different?
LikeLike
Thanks for the question! There is a vaccine for humans. The difference between the vaccine for humans and the vaccine for dogs (for example) is that humans often receive the vaccine only after a potential exposure to rabies, whereas the current policy of preventative vaccination in dogs is one of the reasons rabies in humans is so rare in the U.S. We prefer to vaccinate dogs before possible infection rather than humans because the dog vaccine is much cheaper ($15-20 versus $3000 for the human vaccine), and the relative ease of administration of the dog vaccine in comparison to the human vaccine: the dog vaccine is a single shot given during the first and third years with annual boosters, while the human vaccine is four shots given over a two week period (followed by periodic testing for immunity and boosters given as needed). In short, giving the vaccine in a preventative manner to dogs and cats is much more cost effective and accompanied by lower risk of side-effects than preventative vaccination of humans, while still effectively preventing human infection.
LikeLike
It seems to me that the cost differential (15 for dogs and cats vs 3000 for humans) for what is essentially the same vaccine, and one that hasn’t changed materially since Pasteur created the first 140 years ago, is entirely due to excessive patent abuse and bureaucratic red tape. Otherwise, there’s no reason why every child in America and beyond can’t be offered a preventative dose as part of a normal vaccine regimen for $15. Am I missing something. Shannon? Why else is there such a cost difference?
LikeLike
Well written summary
LikeLike
The rabies infection case is rarely found in the U.S., comparing to that found in the tropical Asian countries like Thailand. Currently, Thailand is now suffering from rabies virus outbreak and 6 fatal cases from this disease have been reported so far. the number is still on the rise. Therefore, get a pre-exposure prophylactic vaccine before planning your trip to Thailand.
LikeLike