Written by: Gabrielle Huizinga
Editors: William Dean, Rebecca Dzombak, and Noah Steinfeld
SARS-CoV-2, the virus that causes COVID-19, first emerged in Wuhan, China in December 2019 and quickly spread to the United States beginning in January 2020. At the time of writing, there have been over 39 million cases worldwide with a fatality rate around 2.8%. While hospitals and public health officials are primarily concerned with the short-term effects of COVID-19, such as hospitalization rates, shortages of supplies, and the spread of the virus, many viruses can cause long-term illness. There have already been reports that people who have recovered from COVID-19 experience lingering myocarditis, or inflammation of the heart muscle. This can cause the heart to not function properly and puts excess strain on the body. Patients infected in the 2003 outbreak of SARS, a virus similar to SARS-CoV-2, experience chronic illnesses, such as chronic fatigue syndrome, abnormal lung function, and decreased exercise capacity. Our ability to understand the long-term effects of a newly-emerged virus like SARS-CoV-2 are limited, but the long-term symptoms of similar, more well-understood viruses may be informative when thinking about why we need to take action now to limit the spread of the disease through increased sanitization, the wearing of face coverings, and minimizing contact with others.
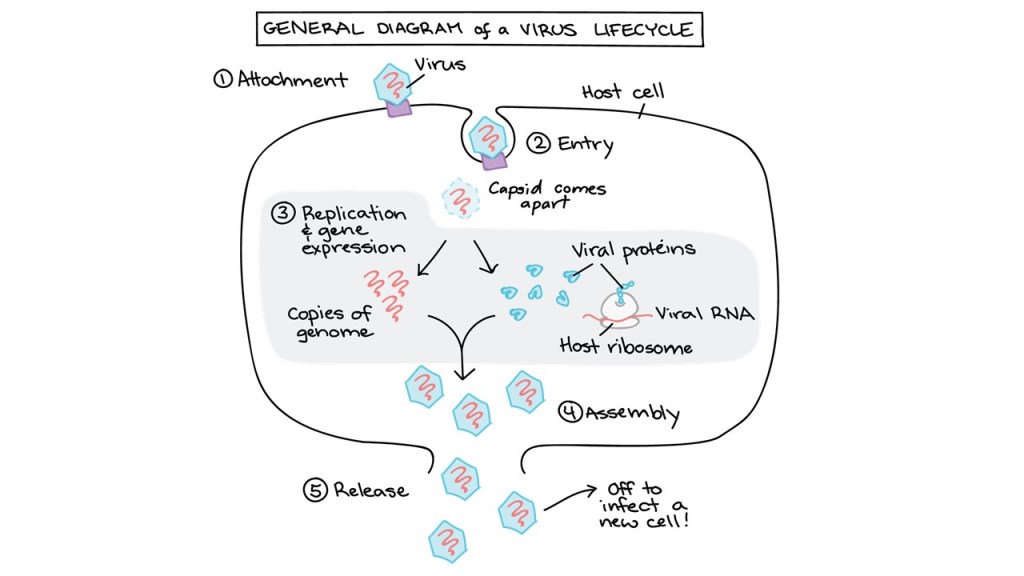
Unlike human cells, viruses cannot replicate on their own. Instead, they must infect and hijack the replication machinery in the human host cell (Figure 1). Viruses carry proteins on the surface of their capsules that bind to receptors on host cells. The spike protein on the viral envelope of SARS-CoV-2 attaches to a cell surface protein that is found in many areas of the body, including the lungs, fat, intestines, kidneys, and brain. This binding triggers the host cell to bring the virus inside the cell. Once inside the host cell, the virus sheds its lipid envelope or capsid and begins to reproduce. Over time, the virus creates many copies of itself. Like with some other viruses, once the host cell is too full of virus particles, SARS-CoV-2 kills the cells, causing them to burst, resulting in damage that causes the short-term symptoms of the disease. For SARS-CoV-2, this cell damage leads to a wide variety of symptoms, including fever, cough, shortness of breath, and GI symptoms. Burst cells will release virus particles into the body to infect other cells, until the body’s immune system can attack and kill the virally infected cells. Even once the virus is removed from the body, long-term effects can still arise from permanent tissue damage. For SARS-CoV-2, some patients have already experienced severe organ damage, including acute respiratory distress syndrome, blood clots, and acute kidney damage. These damages can be deadly not only in the short term but possibly years into the future if the organs do not recover and are permanently impaired. It will be important to follow up with COVID-19 patients regularly to assess organ function and determine any long-term pathology to specific organs.
In addition to regular follow-ups with patients, we can use lessons from more well-studied viruses to help guide our thinking about the kinds of long-term effects SARS-CoV-2 may have. The Human Immunodeficiency Virus (HIV) is the virus that causes Acquired Immunodeficiency Syndrome (AIDS). Unlike SARS-CoV-2, HIV is a retrovirus that infects CD4+ T cells. These cells are a part of the immune system and are important in recognizing viruses and bacteria in the body. Over the course of an HIV infection, the body’s T cells are destroyed, leading to an increased risk of infection and cancer. SARS-CoV-2 destroys lung cells, which may also lead to an increased risk of later severe lung infections. Only time will tell how this destruction will affect lung function throughout a patient’s lifespan.
The varicella-zoster virus is the causative agent of chickenpox. While most people think of chickenpox as an itchy rash that can be easily prevented by vaccines, it is a highly contagious virus that can linger in your body for years after infection. While most cases of chickenpox clear within 21 days, the virus can live inside nerve cells for many years. As we age, our immune system weakens. This allows the virus to emerge from latency and cause shingles, which are painful blisters. We know that SARS-CoV-2 is present in stool samples of children up to 21 days after their nasal swabs show no evidence of the virus. However, we don’t know if the virus continues to hide in other cells in the body. It is possible that the virus can be reactivated during normal aging, possibly causing damage outside of the lungs where it first infects.
The Human Papilloma Virus (HPV) is a virus that causes warts on the skin or in mucus membranes. There are over 200 different types of HPV, and while most are benign or only cause warts, some types can cause cancer (e.g., cervical cancer). While the immune system is typically able to clear the virus within a few days to weeks after infection, some types, especially those that cause cancer, may persist for decades. These persistent strains of HPV can interfere with the body’s natural anti-cancer mechanisms. It is currently an active area of study to determine if SARS-CoV-2 can act similarly.
Although different viruses function differently within the human body, we can learn important lessons from other viruses when thinking about how to combat SARS-CoV-2. It is concerning that viruses can have long term effects through damage to the immune system, living latently in our body, and causing cancer. However, with the wearing of face coverings and limiting social gatherings, we can stop the spread of the virus and minimize both short-term and long-term illness. Many younger individuals may see a low death rate for their age group as a sign to live life normally. However, with concerns that any infection may be a ticking time bomb for later health problems, it is critically important for younger people to take serious precautions. Only time will tell what the full extent of the public health effects of this pandemic will be.

Gabrielle (Gabby) Huizinga completed her undergraduate degrees in microbiology and molecular genomics & genetics at Michigan State University. She is a member of the PIBS class of 2019 and joined the Immunology Graduate Program in April 2020. She is a second-year graduate student in the Immunology Graduate Program working with Dr. Durga Singer and Dr. Beth Moore to pursue her PhD. She is also completing the Diversity, Equity, and Inclusion certificate. Her thesis project aims to understand how obesity affects macrophages and their response to bacterial infection. She is also interested in how sex differences, especially during obesity, affect the immune system’s response to infection.
